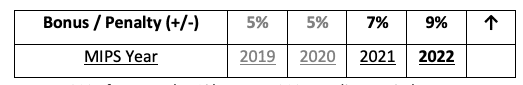The Merit-based Incentive Payment System (MIPS) is the subset of rules under the Medicare Access and CHIP Reauthorization 
Presently, providers may choose to use an Alternative Payment Model (APM) instead of MIPS. The goals of MACRA
The Impacts of COVID-19
The future of healthcare remains uncertain amid ongoing concerns and COVID-19. Following the lockdowns of 2020, CMS relaxed MIPS requirements and offered exemption from reporting. In November 2021, CMS announced it would extend similar COVID-19 related exemptions for the 2021 calendar year in the Final Rule as well. While ripple effects from the pandemic will likely be felt for years to come, banking on a third year of exemptions in 2022 would be risky and not advisable.
Coming Up
This post is the first in a multi-part series intended to assist healthcare administrators and medical providers better understand major changes in our national health system. Our next post will cover specific changes with Quality and Cost standards in 2022 reporting.
To learn more, please stay tuned as Bright Ideas Medical Consulting will keep you in the know.